You have 847 pages of medical records. Your deposition is in three days. Without a properly structured medical chronology, you are not just disorganized — you are handing the opposing counsel an advantage.
A well-built medical chronology does more than sort events by date. In litigation, it becomes the backbone of your case narrative — connecting injuries to incidents, treatments to damages, and providers to opinions. It is the document that turns complex medical records into a compelling, court-ready story.
In this guide, you will get a free, attorney-tested medical chronology example template (Word, PDF, and Excel formats), a step-by-step breakdown of how to use it effectively in medico-legal cases, and a real-world case study from MRR Health Tech’s review team — a delayed stroke diagnosis that illustrates exactly how a structured chronology surfaces the failures buried across fragmented records.
What You’ll Learn in This Guide
- What a medical chronology template is and why it matters in litigation
- The exact fields your template must include (with a free sample)
- When to use Word, PDF, or Excel formats and why
- A real delayed stroke diagnosis case study — how MRR’s chronology exposed five critical timeline failures in ER documentation
- When to build in-house vs. when to outsource to professionals
What Is a Medical Chronology Template and Why Does It Matter in Litigation?
A medical chronology template is a structured, date-ordered document that captures every clinically and legally significant event in a patient’s medical history — from the date of injury through the most recent treatment.
In medico-legal contexts, it transforms scattered medical records from dozens of providers into a single, navigable timeline. But here is the critical nuance most generic templates miss: a medical chronology built for litigation is not the same as a clinical patient summary. It must be filtered through the lens of legal relevance.
Why Attorneys Cannot Afford a Poorly Built Chronology
A missing provider visit, an incorrectly sequenced treatment, or a vague entry can undermine your entire damages narrative. According to the American Bar Association, disorganized medical records are one of the top three reasons personal injury cases settle below value.
A properly structured medical chronology example template eliminates that risk. It creates a verifiable, source-linked timeline that withstands scrutiny at every stage — demand, mediation, deposition, or trial.
What a Medical Chronology Is NOT
Each of those documents serves a distinct purpose. Internal links: see our dedicated pages on Narrative Medical Summary Services and Billing Summary Services for how they work alongside the chronology in a complete case package.
The Essential Fields in a Litigation-Ready Medical Chronology Template
Most free templates you find online were built for clinical or administrative use. They lack the fields that make a chronology useful inside a legal workflow. Here is exactly what your template needs to capture.
Core Required Fields
| Field | Why It Matters in Litigation |
| Date of Service | Establishes causal chain — every gap or continuity in treatment tells a story |
| Provider Name & Specialty | Critical for deposing witnesses and identifying treating vs. retained experts |
| Facility / Location | Jurisdiction relevance; identifies in-network vs. out-of-network billing issues |
| Chief Complaint / Diagnosis | Links injury to event; ICD-10 codes support damages calculations |
| Treatment / Findings | Documents what was done, prescribed, or recommended — forms basis of disability narrative |
| Medications Prescribed | Supports pain and suffering claims; flags opioid use or pre-existing conditions |
| Source Document / Bates | Every entry must be traceable; opposing counsel will challenge unsourced entries |
| Reviewer Notes (optional) | Internal flag for inconsistencies, provider conflicts, or follow-up needed |
Free Medical Chronology Example Template (Word, PDF & Excel)
Below is MRR Health Tech’s attorney-tested medical chronology example template. It is pre-structured for personal injury, workers’ compensation, and medical malpractice cases — the three most common medico-legal practice areas.
Sample: Medical Chronology Example Template
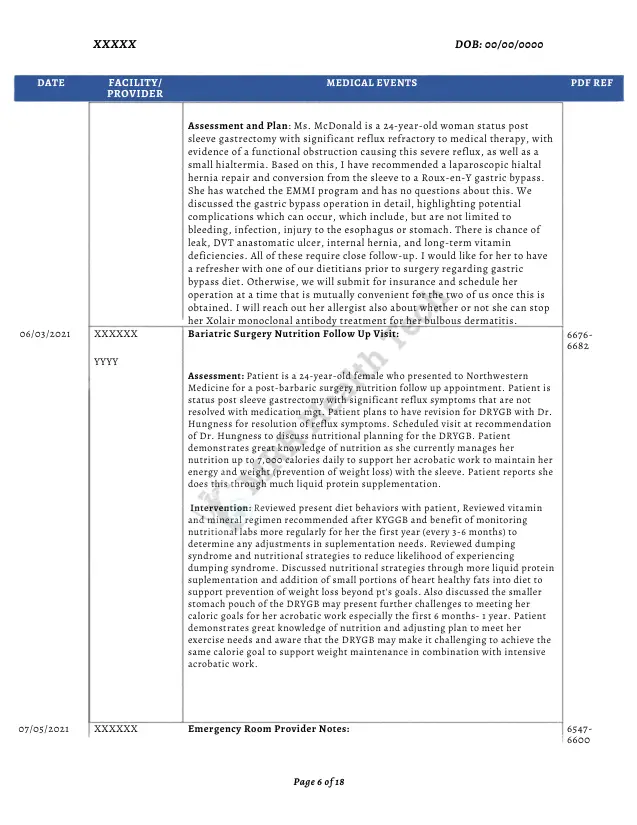
Want More Medical Chronology Samples?
Check out our sample chronology prepared by our licensed medical team on your actual case records
Word vs PDF vs Excel: Which Medical Chronology Template Format Should You Use?
Search intent data tells us attorneys look specifically for ‘medical chronology example template Word,’ ‘medical chronology example template PDF,’ and ‘medical chronology example template Excel.’ Each format has a distinct role in the litigation workflow — here is when to use each:
| Format | Best For | Pros | Cons |
| Word (.docx | Initial drafting & attorney edits | Easy to edit, comment, track changes | Version control can get messy |
| Excel (.xlsx) | Large record volumes, filtering | Sortable, filterable, date-searchable | Less readable for narrative notes |
| Final submission, court filing | Tamper-evident, universally readable | Not editable after export |
Pro Tip: Start in Word or Excel for the drafting phase. Use PDF only for final submission, court filing, or sharing with opposing counsel. Never send an editable chronology to external parties unless intentional.
Real Case Study: How MRR’s Chronology Exposed a Delayed Stroke Diagnosis
MRR Health Tech Case Study | Reviewed by MRR Medical Review Team
- Practice Area: Medical Negligence – Emergency Department / Delayed Stroke Diagnosis
- Case Type: Neurological Injury / Ischemic Stroke
| Case Type | Medical Negligence – Delayed Stroke Diagnosis (ER Setting) |
| Client | Plaintiff’s Attorney (name withheld) |
| Patient | Middle-aged female, presented to Emergency Department |
| Records Reviewed | ER triage notes, nursing documentation, physician assessments, imaging reports, neurology consultation records |
| Core Issue | Failure to recognize classic stroke symptoms; no stroke alert activation; delayed imaging and specialist consultation |
| MRR Deliverable | Structured chronology correlating symptom progression, nursing observations, physician responses, and imaging delays |
| Outcome | Timeline clearly established that earlier recognition and intervention could have reduced severity of permanent neurologic deficits |
The Problem: Classic Stroke Symptoms, Missed at Every Escalation Point
A middle-aged female patient presented to the Emergency Department reporting headache and dizziness. During triage, she also mentioned left-sided weakness. Within hours, she developed facial drooping — one of the most recognizable hallmark signs of acute stroke.
Despite these documented neurologic complaints appearing across multiple record types, the ER response failed at every critical escalation point:
- No stroke alert was activated despite documented neurologic symptoms
- The neurological examination was delayed — NIH Stroke Scale was never documented
- CT imaging was not ordered promptly; the delay was not explained in physician notes
- Symptoms were attributed to headache, vertigo, and dehydration — not a neurologic emergency
- The patient was left for several hours without a neurology consultation
What made this case particularly significant from a litigation standpoint was a documentation conflict that MRR’s reviewers identified: the handwritten nursing notes described worsening weakness and confusion at multiple reassessment intervals — yet the physician progress notes continued to record the patient as “stable.” That contradiction, buried across separate documentation streams, was invisible without a structured chronological review.
MRI imaging obtained at a later stage confirmed ischemic stroke involving the middle cerebral artery — a diagnosis that could have been reached hours earlier based on the symptoms already documented in the record.
The MRR Health Tech Review Process
MRR’s medical review team — comprising a licensed physician and certified medico-legal analysts — conducted a comprehensive, litigation-focused review of all records. The scope of review included:
Critical Timeline Failures Identified
MRR’s review identified five distinct, source-linked failure points within the medical record:
| Failure Point | Evidence in the Medical Record |
| Missed recognition of stroke symptoms | Triage note documented left-sided weakness + facial drooping; no stroke protocol initiated |
| Failure to document ‘Last Known Well’ | Critical timing for tPA eligibility was never established in any physician note |
| Delayed emergent imaging | CT imaging ordered hours after initial neurologic complaints; no documented rationale for delay |
| Delayed emergent imaging | Neurology not notified until significant deterioration; nursing re-assessments noted worsening during this gap |
| Missed therapeutic intervention window | tPA was never administered; documentation confirms patient was within the treatment window at initial presentation |
The MRR Chronology Deliverable
MRR developed a concise, source-linked medical chronology that correlated five streams of documentation into a single, litigation-ready timeline:
- Symptom Progression: From initial triage complaint through documented neurologic deterioration
- Nursing Observations vs. Physician Response: Side-by-side mapping of nursing-documented worsening against physician-recorded ‘stable’ status — the core contradiction in the case
- Imaging Delay Timeline: Timestamped order-to-result gap demonstrating the window in which intervention was possible
- Consultation Gap: Time elapsed between first documented neurologic symptom and neurology notification
- Therapeutic Window Analysis: Clinical notation confirming the patient’s eligibility for tPA at the time of presentation, cross-referenced against the actual time of MRI confirmation
What the Chronology Established for Litigation
The completed chronology made visible what fragmented records had concealed: a progressive, recognizable neurologic emergency that was not appropriately escalated or treated.
The timeline clearly supported the argument that earlier recognition — at any of the five identified failure points — could have resulted in timely imaging, prompt neurology consultation, and tPA administration within the therapeutic window, likely reducing the severity of the patient’s permanent neurologic deficits.
Key Takeaway for Attorneys
In delayed stroke diagnosis cases, the evidence is almost always present in the record. It is simply not visible until it is organized. The nursing notes documented the deterioration. The imaging reports confirmed the injury. The medication records showed the missed window. What was missing was a single, structured chronology that connected all of it — in sequence, with sources, in language an expert witness, mediator, or jury can follow.
That is exactly what MRR’s medical chronology services deliver.
Step-by-Step: How to Use a Medical Chronology Template in Litigation
Step 1 — Collect and Organize All Source Records
Before you open the template, gather every record. Do not begin data entry on incomplete documentation. Missing records discovered mid-chronology mean resequencing and re-sourcing — wasted time with HIPAA and re-authorization risks.
Record types to collect for a complete medico-legal chronology:
- Emergency room records and ambulance/EMS run sheets
- All treating provider notes (primary care, specialists, surgeons)
- Imaging studies and radiology reports (X-ray, MRI, CT, ultrasound)
- Laboratory results and pathology reports
- Physical, occupational, and speech therapy notes
- Operative reports and anesthesia records
- Mental health and neuropsychological evaluations
- Pharmacy records and prescription history
- Insurance authorizations and denial letters (critical for gap explanations)
- Employer records and functional capacity evaluations (FCE)
Step 2 — Bates-Stamp and Index All Records
If your records are not already Bates-stamped, do it before you start the chronology. Every chronology entry must reference a specific page or range. This is non-negotiable for litigation use — opposing counsel will request source documentation for every entry at deposition.
Step 3 — Populate the Template Chronologically
Enter events oldest to newest using exact dates from the source documents. If a document contains only a month and year, note it as ‘circa [Month Year]’ and flag for verification. Do not estimate or approximate dates without annotation.
Write event descriptions in factual, neutral language:
Language Examples
- ✔ Correct: “Patient presented with cervical pain rated 7/10. MRI ordered”
- ✘ Avoid: “Patient suffering from serious neck injury caused by negligent driver”
Advocacy language belongs in your narrative summary and demand letter — not in the chronology.
Step 4 — Flag Gaps, Inconsistencies, and Key Events
After the first-pass population, review the complete timeline for:
Step 5 — Export to the Right Format
Working draft: Stay in Word or Excel. Final submission or sharing with opposing counsel: Export to PDF. For court filing, ensure the PDF is text-searchable (not a scanned image).
7 Most Common Medical Chronology Mistakes Attorneys Make (And How to Fix Them)
DIY Template vs. Professional Medical Records Review: Which Approach Is Right for Your Case?
The honest answer: it depends on case complexity and the resources your firm has. Here is a practical decision framework:
| Factor | DIY Template | Professional Review (MRR Health Tech) |
| Case Complexity | Simple soft-tissue, low record volume | Multi-provider, >200 pages, disputed causation |
| Time Available | 2+ weeks to complete internally | Need results in 24–72 hours |
| Medical Terminology | Paralegal or attorney confident with clinical records | Complex diagnostic language, specialist records |
| Stakes | Small claims, early resolution | High-value litigation, trial, or expert deposition |
| HIPAA Handling | Internal protocols in place | Certified external review with BAA in place |
| Cost Sensitivity | Tight budget, straightforward case | Cost-per-case justified by settlement value increase |
For cases involving disputed causation, multiple providers, injuries spanning more than six months, or where expert testimony is anticipated, the cost of professional medical records review is almost always recovered in the settlement or verdict improvement.
MRR Health Tech’s medical chronology services include source-linked timelines built by licensed physicians and certified medical coders, with turnaround times starting at 24 hours. See our Medical Chronology Services page for sample deliverables and pricing.
Frequently Asked Questions About Medical Chronology Templates
What is the difference between a medical chronology and a medical summary?
A medical chronology is a date-ordered table of events, neutral in tone, linked to source documents. A medical summary (or narrative summary) is a prose document that interprets those events in a clinically coherent narrative — it explains what happened and why it matters. In litigation, you typically need both. The chronology supports the summary; the summary supports the demand.
Can I use a free medical record example PDF as a template?
You can use it as a reference for structure, but most generic medical record examples are built for clinical use, not litigation. They typically lack Bates number fields, legal source references, gap notation, and litigation-specific event descriptions. Always adapt any template to include the eight core fields outlined in Section 2 of this guide before using it on an active case.
How long does it take to build a medical chronology?
Internal time estimates vary widely by record volume and complexity. For a typical 200-page personal injury file, expect 8–12 hours of paralegal time to produce an adequate chronology. For 800+ page files with multiple providers and complex medical terminology, internal preparation can exceed 30–40 hours. MRR Health Tech’s professional team typically delivers the same file in 24–48 hours.
Conclusion: The Right Template Is Just the Starting Point
A medical chronology example template — whether in Word, PDF, or Excel format — gives you a framework. What you fill it with determines whether it helps or hurts your case.
The most effective chronologies in litigation share three characteristics: they are complete (every record, every provider, every gap explained), they are source-linked (every entry traceable to a specific page), and they are clinically accurate (no misread diagnoses, no understated severity, no missed findings).
For straightforward cases with manageable record volumes, the template in this guide gives your team everything needed to build a solid, litigation-ready timeline. Download it, adapt it to your practice area, and use the step-by-step guidance to ensure nothing is missed.
For high-value cases, complex multi-provider files, or situations where clinical accuracy is case-critical, MRR Health Tech’s medical review team delivers professionally prepared chronologies with the expertise of licensed physicians and certified coders — typically in 24–48 hours.
Ready to Build a Stronger Case? Start With a Free Trial!
MRR Health Tech’s medical review team has helped attorneys across the USA prepare chronologies, narrative summaries, billing reviews, and demand letters. Submit Your Case for a Free Trial!
About the Author
MRR Health Tech Medical Review Team
This article was researched and written by MRR Health Tech’s in-house medical review team — a multidisciplinary group of licensed physicians, certified medical coders (CPC), and medico-legal analysts with combined experience reviewing medical records for attorneys across all 50 U.S. states.
MRR Health Tech specializes in medical records review for plaintiff and defense attorneys handling personal injury, workers’ compensation, medical malpractice, and mass tort litigation. Our team has reviewed over 50,000 cases and currently supports law firms in all 50 states.
Website: medicalrecordsreview.com | Email: review@medicalrecordsreview.com | Phone: +15302400250



